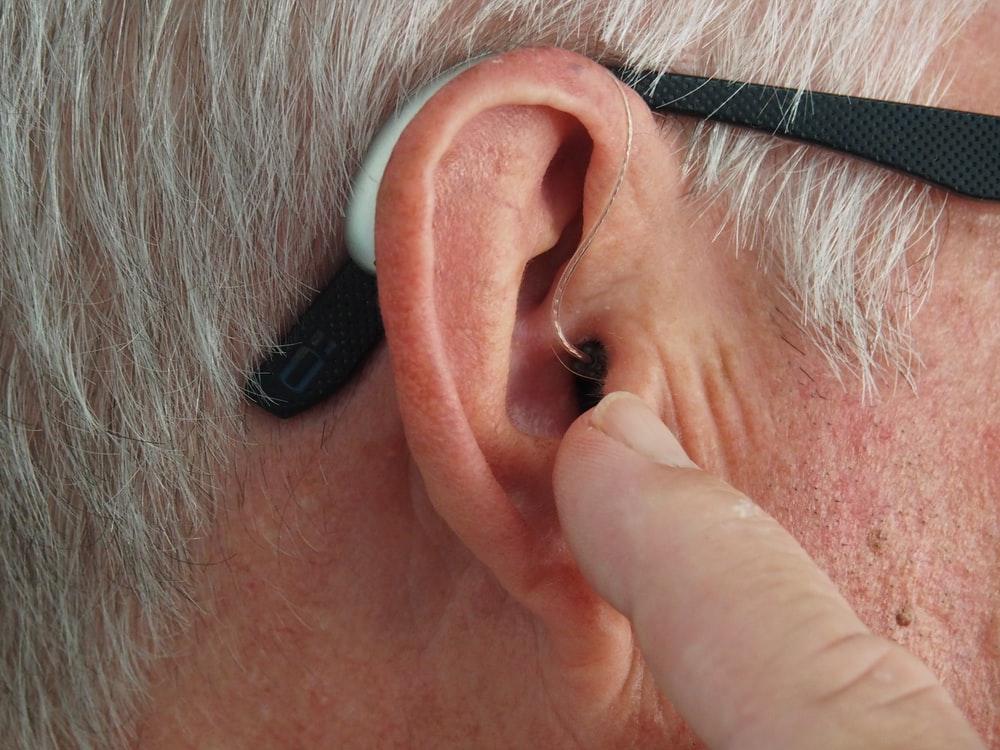
Ear eczema, commonly known as atopic dermatitis, is an inflammatory skin condition. It forms a scaly, red, and itchy rash called eczema on the skin’s surface. Ankles, feet, inner elbows, eyeballs, and the inside and outside of the ears are just a few body parts that may be affected by this condition. Eczema in ears may bring several difficulties and some distinct symptoms and problems.
What is Ear Eczema?
Eczema in ears is a skin disorder that causes discolouration, dryness, and itching in, on, and around the ears. Although it is not communicable, it is more likely to develop if you have a genetic history of eczema, asthma, or allergies.
Types of Ear Eczema
Ear eczema pain comes in different types. In addition, each array of ear eczema has a distinct set of triggers. Let’s know about these six types of eczema that may affect your ears.
1. Atopic eczema
Atopic eczema patients have more sensitive skin than the average person. This results in dry, itchy skin that may get infectious if the skin cracks. Eczema in ears of this kind develops when the skin loses its ability to retain moisture and cracks open. In addition, it may cause allergic reactions to the ear canal. The most typical location for atopic eczema to appear is behind or around the ear lobe.
2. Irritant contact dermatitis
The most prevalent kind is irritant contact dermatitis. A chemical damages your skin’s outer protective layer, causing fluid to flow from blood vessels. This fluid causes the skin to become red, swollen and itchy.
Some persons have an allergic reaction to powerful irritants after just one encounter. Even modest irritants might cause symptoms in some people with repeated contact. Some people become accustomed to the chemical and no longer require it.
This condition is known as allergic contact dermatitis, and it happens when your skin’s immune system reacts abnormally to an allergen. It usually affects just the region that comes into touch with the allergen. However, food, flavours, medicines, dentistry, or medical treatments (systemic contact dermatitis) might set it off.
3. Allergic contact dermatitis
Your body’s immune system reacts whenever it comes into touch with an allergenic that it does not like. Inflammatory mediators are released by white blood cells that have been drawn to the skin. The rash becomes itchy as a result of this reaction. The rash may occur minutes, hours, or even days later, depending on exposure. Allergy to poison ivy is one of the most common causes of contact dermatitis.
4. Otitis externa
Otitis externa is an infection of the external auditory canal, typically caused by bacteria. It may also be caused by noninfectious local or systemic dermatitis processes. The most common symptom is pain, followed by erythema and edema of the canal with varying discharge.
Excessive humidity and trauma, which impair the canal’s natural protection, are common causes of otitis externa, and minimizing these precipitants is an important part of prophylaxis. In order to adequately identify and treat the problem, the canal must also be thoroughly cleaned. Flushing, on the other hand, is not advised. It is possible to effectively cure inflammation and prevent it in the future by using a topical solution of 2% acetic acid and 1% hydrocortisone after exposure to moisture.
5. Seborrhoeic dermatitis
Most people with seborrheic dermatitis experience it on their scalp. Scaly spots, red skin, and persistent dandruff are all symptoms of the condition. Those with seborrheic dermatitis may also have oily regions of the body, including the cheeks, sides of the nose, and the eyebrows.
Seborrheic dermatitis may fade away if it is not treated. Alternatively, it may take longer for the symptoms to go gone. But they may return at some point. Regular cleaning with mild soap and shampoo may help minimise the appearance of oiliness and dead skin cells.
6. Asteatotic eczema
Seborrheic dermatitis is also known as dandelion dermatitis, eczema, and psoriasis. In addition, crotch-scaly patches appear on the scalp of babies with the ailment known as cradle cap.
Eczema characterised by dry, itchy, and cracked skin is known as asteatotic, although known as xerotic, or simply “eczema craquelé.” It’s more frequent in the elderly, although it’s not unheard of among persons in their twenties. The lower legs, thighs, chest, and arms are the most typical places to see red, flaky patches.
Most people have symptoms during the winter months, especially in regions where interior humidity levels are reduced due to heating systems. However, a warm, humid temperature may help alleviate symptoms of this skin disease, both inside and out.
Signs and Symptoms of ear Eczema

Eczema that becomes infected is more likely due to skin fissures caused by itching and dryness. In addition, a buildup of hair and skin in the ear canal might cause ear eczema infection or poor hearing. Eczema in the ears may cause the following ear eczema symptoms:
- Itchy, red, and irritated skin.
- Itchy skin.
- Discoloured skin rashes.
- Bumpy skin.
- Scaly, leather-like areas.
- Rusty, flaky skin.
- Swelling.
Eczema of the ear is not painful. As a result, you must avoid scratching your ear eczema pain to prevent infection, which may cause discomfort.
Treating Ear Eczema
Before treating it, you know why you’re experiencing the ear eczema symptoms. First, find out what causes or aggravates your ear eczema, and afterwards, stay away from it. This ear eczema treatment is implemented to lessen the pain and itching and avoid ear eczema infection and further flare-ups.
Eczema in the ears may be relieved with the help of these at-home remedies:
- Nickel, cobalt, and copper earrings, for example, are frequent allergies to avoid.
- If dry air causes your skin to get irritated.
- Keep your ears toasty when it’s chilly outside by donning a hat.
- Make sure you don’t irritate or scrape your skin.
- Take hydrocortisone ointment or cream. Hydrocortisone is a combination of a corticosteroid and an analgesic. It reduces redness and blemishes.
- Apply a lotion or ointment to your skin to keep it hydrated. Unfortunately, they don’t always function as well. You should use it multiple times a day, especially after a shower or bath. Hydration is maintained by using a moisturiser.
- Take a lukewarm bath or shower rather than a hot one. Wash your ears gently. Do not spend any more than 15 minutes in the water at any one time.
- Do not use perfumes, dyes, or alcohol-based hair and skin products. Instead, fragrance-free, hypoallergenic and sensitive skin-friendly goods are the ones to look for.
- Launder your garments with mild soap and then thoroughly rinse them.
- Use ceramide-containing skincare products. These products may be able to repair the “glue” (the barrier) that has been removed from your skin. Cotton clothing is best. Fabrics such as wool, silk, and others may irritate and dehydrate the skin.
- Take antihistamines over the counter (OTC) if you’re experiencing extreme itching.
- Your doctor may prescribe steroid creams, tablets, injections, or ear drops. The long-term hazards include side effects such as increased blood pressure, weight gain, and skin thinning. However, topical immunomodulators (TIMs) have shown promising results in treating individuals who have previously failed to react to conventional therapy. They alter the body’s immune reaction to allergens and are less likely to cause adverse effects.
- Consider using the healing powers of light. For example, a particular bulb emits UVB light used in phototherapy. In addition, sunlight’s UV rays may help treat various skin conditions, including eczema.
Prevention Tips for Ear Eczema
There are things you may do to help avoid ear eczema outbreaks, including the following:
- Establish a skincare regimen and adhere to your healthcare provider’s instructions to maintain your skin healthy.
- You should avoid wool and silk since they might dry out the skin.
- Bathe or shower with a gentle soap bar, then pat rather than rub the water off your skin. To assist keep moisture in your skin after drying it, use a moisturising lotion or ointment soon after drying it. Reapply the lotion or ointment every two to three hours.
- Take lukewarm baths or showers rather than heated ones.
- Ensure that you consume at least eight glasses of water every day. Water aids in the preservation of moisture in the skin.
- Avoid temperature and humidity swings that are too abrupt.
- Keep your exposure to recognised irritants and allergies to a bare minimum.
- If you have itchy skin, try not to scratch or massage it.
Conclusion
Ear eczema isn’t generally life-threatening, although it may be bothersome. However, the itching and dry skin may be aggravating, and scratching can exacerbate these symptoms. In addition, people with eczema in the ear canal are more likely to have ear eczema infections.
However, eczema is usually cleared up with appropriate ear eczema treatment, and there are no long-term repercussions. Home treatments and lifestyle adjustments are generally sufficient for most individuals who suffer from ear eczema to keep it under control.
FAQs
How contagious is ear eczema?
It isn’t infectious. Skin-to-skin contact cannot spread ear eczema.
How to detect ear eczema?
Your doctor will check your ears. They’ll search for ear eczema symptoms, including discolouration and dryness. An otoscope is used to see into your ear. And about your symptoms.
Do I need to take any precautions?
Ear eczema pain is often treatable with good skincare and therapy. However, symptoms might flare up at any time in your life.
Is ear eczema curable?
Ear eczema is a chronic illness with no ear eczema treatment. However, treatments for dry, itchy skin are often successful.
What are my options for self-care?
Ear eczema is common. But it’s not always easy.
Your ear eczema may go away at times. These are “remission” times. However, prolonged use of a lousy skincare regimen might cause flare-ups. Avoid things that cause ear eczema, moisturise, take your medication, and listen to your doctor.